Preparing Mangochi District Hospital for the COVID-19 Epidemic
|
The COVID 19 epidemic has overwhelmed healthcare systems, challenged supply chains and thrust infection control to the forefront of the response throughout the world. Preparing the healthcare system in Malawi has been a herculean multi-disciplinary effort throughout agencies, government and implementing partners. At the nexus between the COVID 19 prevention and treatment efforts and the community these efforts are intended to serve, are the people of the health care facility itself. The following story outlines the rapid response to prepare Mangochi District Hospital, and the collaborative and determined spirit of the people that made it possible.
Baylor College of Medicine Children’s Foundation Malawi (Baylor) has been an integral stakeholder supporting Mangochi District Hospital’s preparation for COVID 19 in three main areas: infection prevention through establishing hand hygiene stations and provision of PPE; establishing a screening and triage protocol and making physical changes to the facility, including setting up an isolation ward. |
Mangochi District Hospital is an integrated health facility serving one of Malawi’s most populous districts. It is also a district with a significant number of migrant fisher people, farmers and ex patriot laborers in South Africa, with frequent travel across porous borders, such as with Mozambique. Mangochi District Hospital is the largest of the health facilities in the district currently serving more than 8,000 ART clients, with over 30 Baylor staff complementing the ministry staff contingent at the site, from the pharmacy, lab and ART clinic itself.
Baylor is an active member of the District Rapid Response team, and as part of the rapid response assisted the MOH hospital team at the largest referral hospital in the district, to identify the old disused TB ward as the best site for a COVID-19 isolation ward.
At the time that the COVID emergency was declared, the hospital had very few resources for hand hygiene and very little PPE. The hospital experienced outages of water several times per day, and even when water was available, many basins in the wards were not functional and the hospital had no hand soap. Mr. Rashid, the Chairperson of the Rapid Response Team, reflects, “Baylor has helped us with our infrared thermometers, some screening tents… and also in terms of setting up the isolation ward, it's been Baylor. Baylor has also provided us with us a handwashing soap, glove and buckets, just to mention a few. So, I can say Baylor has done a lot in terms of COVID response in Mangochi."
Baylor was the first implementing partner to provide hygiene support to the health facility and within two days of the emergency declared, Baylor had put 42 buckets and basins and soap through-out the hospital in all identified key location. Baylor also used its resources for monthly facility meetings to instead orientate all hospital staff on COVID-19, and used existing weekly forums to emphasize the importance of hand hygiene during the morning report meetings and to monitor its implementation.
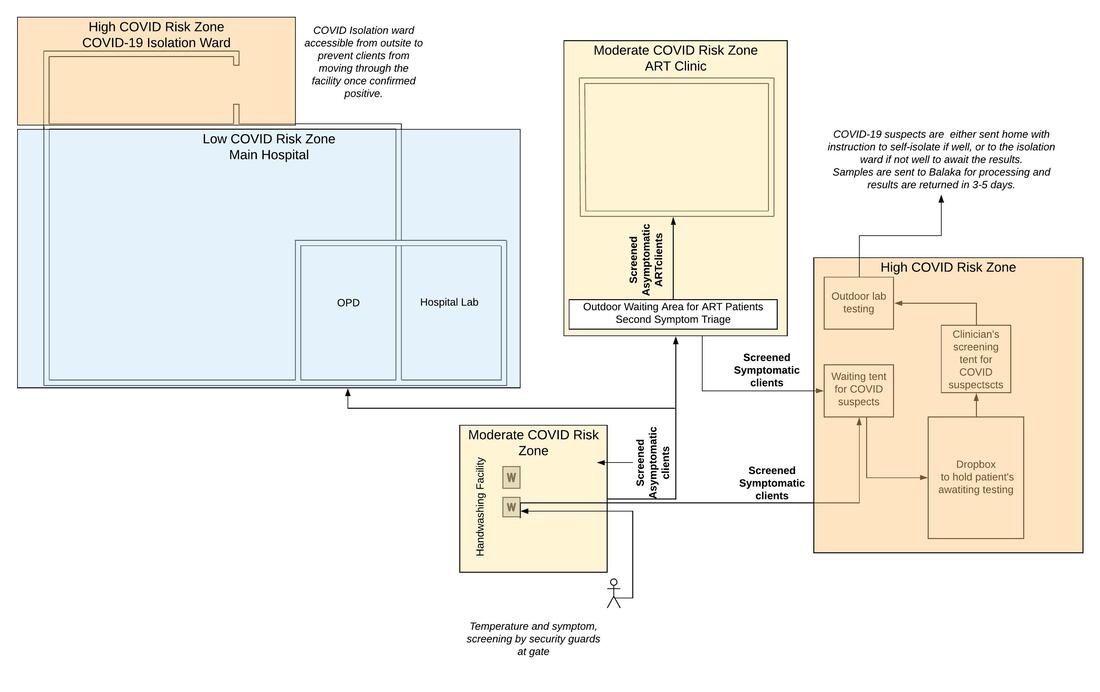
Baylor has also worked hard to facilitate the screening and triage system at the district hospital entrance. According to Mr. Rashid, “I think Baylor has set an algorithm. Now there's a proper referral pathway. In fact, in terms of screening, we now have a clear path. We know that the patients are supposed to go in this direction and maybe those that are supposed to go through the tents.” Baylor facilitated a meeting to finalise triage pathways with stakeholders and provided technical advice. Together with College of Medicine we held two meetings to train 20 HSAs and 15 security guards to conduct screening at the gate and are actively monitoring its implementation daily. We also assisted training of the clinicians who consult the patients who have been screened, including with developing a rota, treatment algorithms and use of PPE. As such the hospital now has a well-functioning screening and triage system.
To ensure that social distancing and infection control measures could be taken as agreed in the triage system, Baylor donated laser thermometers for screening, PPE and a tent that is used to screen all patients with fever and cough before they enter the hospital. Baylor also supported the erection of a larger tent that is used as an outside waiting area for those with fever and cough, and provided fuel to move a “dropbox” previously in disuse, from the back of the hospital to the COVID screening area for those who screen positive and should be isolated while waiting for a provider to test the client for COVID (and TB).
Mr. Rashid notes, “It is Baylor who has that given us the kind of support that we needed as district.” As a result, when the first two COVID suspects were identified, both the ward and staff were ready. These patients were isolated and cared for appropriately without undue fear on the part of the staff, until both test results came back negative.